Cosmetic Non-Surgical Rx Reconstructive Surgical Rx Squamous cell carcinoma Sebaceous cell carcinoma Malignant melanoma Trimalar (tripod) fracture Lacerations |
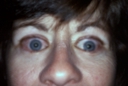
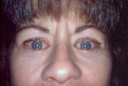
THYROID EYE DISEASE (GRAVES' DISEASE) & EYELID RETRACTIONGENERAL CONSIDERATIONS Hyperthyroidism (overactive thyroid gland) is a condition in which there is overproduction of thyroid hormone. Abnormal antibodies that attack the thyroid gland cause it to become overactive. Abnormal antibodies may also cause swelling and inflammation of the soft tissues around the eyes and the muscles that move the eyes and eyelids. As a result the eyes may protrude, the lids may open too widely, or the eyes may not move together well causing double vision. Therefore, the eyes appear excessively prominent with a staring expression and infrequent blinking. Many patients start experiencing eye problems as soon as their thyroid gland becomes overactive. For some, the eye changes may develop before hyperthyroidism is clinically detected, while others may not develop symptoms until months or years later. Both eyes are usually affected, however they may not be affected to the same degree or at the same time. Some patients may also experience pressure around the eyes, ocular irritation and tearing from excessive exposure of the eyes. Overexposure during the day and difficulty closing the eyes at night can lead to dryness with injury and potential scarring of the cornea (the clear front of the eye). Inflammation of the eye muscles may result in restricted eye movement causing persistent double vision. In some cases these muscles become so swollen that the enlarged muscles can compress the optic nerve resulting in progressive loss of vision. After several months of progressive changes, the active inflammation subsides. Yet, many patients will be left with some degree of residual protrusion, eyelid retraction, or double vision that may require additional treatment. Symptoms referable to exposure can be improved by the use of artificial tears (Refresh eye drops) during the day and lubricant ointment (Lacrilube) at bedtime. Exposure-related symptoms can also be aided by the use of a bedroom humidifier during sleeping hours. When there is active inflammation with more severe symptoms, oral cortisone (steroids) or other anti-inflammatory medications may be needed to reduce the swelling. If muscle swelling around and behind the eye is severe enough, prompt surgery may be necessary to decompress the orbit, thereby protecting the optic nerve from vision loss. SURGICAL TREATMENT In non-emergent cases, surgery for thyroid eye disease is elective. We normally wait until the clinical changes (on examination) have been stabilized and the hyperthyroid status (on thyroid-related blood tests) has been normalized for at least six months. This surgery must be considered in a sequential manner because each surgery affects other manifestations of the disease. In the decision making process, if any surgery is not relevant to the patient, then the next procedure in sequence is considered. The surgical sequence is as follows:
AFTER SURGERY Pain is minimal after surgery and no patch is required. Patients simply use antibiotic ointment at bedtime for approximately 10 days. Ocular lubricants that were used pre-operatively are often continued postoperatively to help maintain corneal protection. Sutures are removed 7 to 10 following surgery in our office RISKS AND COMPLICATIONS Minor bruising or swelling may be expected and will likely go away in one to two weeks. Bleeding and infection, which are potential risks with any surgery, are very uncommon. CONCLUSIONS While it may not be possible to completely eliminate all of the consequences of thyroid eye disease, surgery to correct these conditions is generally quite successful in satisfactorily restoring function, comfort, and cosmetic appearance. |